Insight Survey on Unwinding Data
Check out what NAMD learned from states and territories about the size and scope of their outreach efforts.
Medicaid agencies report expanded outreach and strategies to ensure eligible Medicaid members retain coverage
Medicaid agencies, federal partners, community-based organizations, providers and countless other advocates are working together to ensure that the current redetermination of eligibility for more than 95 million people does everything possible to keep eligible individuals covered and helps people who have become ineligible transition to other sources of health insurance. In support of this, Medicaid agencies across the country have significantly expanded investment in and broadened their member outreach and engagement efforts and are also adopting new federal policy flexibilities that help to streamline renewal processes and protect eligible people in retaining coverage.
All states are actively in process with redeterminations and all are vigilant about learning as much as they can as they gain experience about what strategies are most effective in reaching Medicaid members and ensuring continued coverage for eligible people. This is a very dynamic process and states will continue to adopt new strategies and course correct, as needed, over time. Because of that, it is important not just to look at the initial data that is emerging from early months of the unwinding process, but also where states are situated right now.
For this reason, the National Association of Medicaid Directors surveyed its members – which include all 56 Medicaid Directors from all states, territories and the District of Columbia – to better understand the full scope of the effort those agencies were undertaking. Helpfully, there was a robust response. 34 states and territories responded to the survey providing truly of-the-minute information on their efforts and investments around member outreach as well as use of flexibilities to help eligible members remain covered or, as needed, be restored return to coverage.
Understanding State Outreach and Engagement
The survey posed a number of questions designed to illuminate both the spending and strategies that states are using to connect with members.
States were asked to provide a baseline of funding prior to the pandemic and then provide current outreach funding levels. In response:
- 61 percent of Medicaid programs that responded said they did not have any dedicated funding for member outreach prior to the unwinding, 27 percent said they did and 12 percent lacked the specificity in their budgets to answer the question.
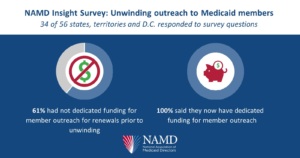
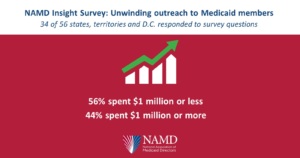
- All Medicaid programs that responded said they have had dedicated funding for member outreach since Congress first required states to maintain eligibility of all people served by Medicaid during the pandemic (the “continuous coverage requirement”). 56 percent have spent $1 million or less and 44 percent have spent $1 million or more on outreach. The size of each state’s population and the expense of placing media had a significant influence on the amount spent to date.
- Nearly every Medicaid program that responded launched a statewide advertising campaign to encourage members to update their contact information, respond to outreach or both.

- 94 percent of Medicaid programs responding are using multiple means to connect with their Medicaid members – through the Medicaid program, providers and managed care organizations — including mail, email, text and translations into additional languages.
- 87 percent of agencies responding said they are leveraging between 8 or more strategies to help Medicaid members stay connected. Strategies surveyed include:
- Advertising campaigns,
- Texting,
- Email,
- Mail,
- Robocalls or outbound calls,
- Outreach through managed care organizations,
- Strategies with sister state agencies,
- Call center enhancements,
- Website enhancements,
- Outreach through community-based organizations,
- Outreach through providers,
- Launch or expansion of community navigator programs,
- Language enhancements like plain language efforts and expanded translations, and
- Community review of notices and specific partnerships with schools.
Understanding how states are using federal flexibilities
CMS has identified a helpful array of flexibilities that states can elect to use to streamline the renewal process and to help ensure that eligible people remain covered. Some of these flexibilities were identified early on in the unwinding process; others have been made available more recently.
A very important example of state use of flexibilities concerns expansion of a provision in federal law that requires that certain Medicaid members have a 90-day window (the “reconsideration period”) within which to return to the program if they have lost coverage but remain eligible. The survey asked states to indicate whether they plan to expand the coverage groups that are eligible for this option as well as strategies that they are using to help Medicaid members understand the process.
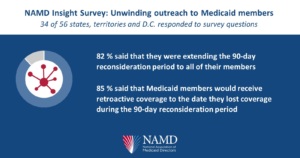
- 82 percent of Medicaid programs that responded said that they were extending the 90-day reconsideration period to all of their members.
- 85 percent of Medicaid programs that responded said that Medicaid members would receive retroactive coverage to the date they lost coverage during the 90-day reconsideration period.
- A majority of the agencies responding said they were engaging in the following efforts or a combination of these efforts during the reconsideration period: Member education about the reconsideration period, outreach to members through navigators and/or community-based organizations, outreach from managed care organizations to members, education for providers about the reconsideration period and reenrollment through managed care organizations. In addition, 13 agencies responding said they were also conducting education about the reconsideration with pharmacies, another location where Medicaid members might first discover they have lost coverage.
States are also interested in and actively considering some of the more recently identified flexibilities. Specifically:
Over 70% of the Medicaid programs that responded to our survey are considering adding between 1 and 4 of the newly available waiver strategies.

- Almost a quarter of the Medicaid programs that responded to our survey (24%) are considering at least 5 additional waiver strategies.
Examples of waivers states are taking up include:
- Renewal of Medicaid eligibility for individuals with income at or below 100% of the Federal Poverty Level for whom no data was returned in the administrative (“ex parte”) review. Many states are considering a strategy that allows for more seamless renewal for very low-income individuals. This permits states to automatically renew an individual’s Medicaid coverage if the state previously determined that they had income at or below 100% of the federal poverty line.
- Reinstate eligibility to the individual’s prior termination date for individuals disenrolled for a procedural reason and then determined to be eligible for Medicaid in the 90-day reconsideration period. This option enables states to reinstate eligibility for a person back to the date on which they lost coverage if they are eligible at the time of submitting a renewal form, as opposed to documenting eligibility as of an earlier date.
- Permit managed care plans to provide assistance to enrollees to complete and submit Medicaid renewal forms. Many states are considering this new flexibility as a means of expanding their capacity to support members.
As all states continue the work of unwinding continuous coverage, NAMD and its members want to emphasize two important points. First, Medicaid programs will continue to do everything possible to support people served by the program in navigating the unwinding process. Second, Medicaid enrollment remains open to all who qualify at any time. Unlike private health insurance, potential Medicaid members do not need to wait for particular qualifying life events or open enrollment periods. We all share the goal of connecting and ensuring continuity of coverage, whether that is through Medicaid, the marketplace or an employer-sponsored insurance plan.
Related resources
How eligibility may look different in this bridging year
NAMD Comments on CMS’s Interim Final Rule on the Medicaid Unwinding
Stay Informed
Drop us your email and we’ll keep you up-to-date on Medicaid issues.